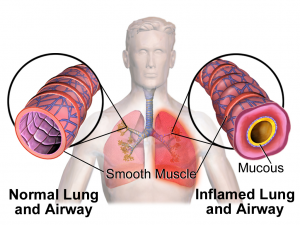
Asthma is a chronic condition characterized by variable airflow obstruction, air passage inflammation and hyper-responsiveness to stimuli. When triggered, the airways become more swollen, and the muscles around the airways tighten up, making it hard for air to move in and out of the lungs. Long term inflammation and injury to the airway linings cause more structural changes leading to worsening symptoms and lung function decline.
Asthma, like many other allergic diseases, tends to run in the family. Many people’s asthma is triggered by allergies. However, lots of people without allergies can also have asthma. Common triggers include exercise, virus infections, smoke, temperature and humidity changes, air pollution, strong smells, emotions, etc. People doing certain jobs may develop occupational asthma.
Symptoms
The most common symptom of asthma is wheezing. However, it can present with other symptoms such as shortness of breath, chest tightness, chronic cough, night time awakening due to cough or wheezing, easy fatigue or cough with exercise.
Diagnosis
After taking a thorough medical history, your doctor may order a breathing test to look at how your lungs work. A common test is called spirometry, which is usually performed in your doctor’s office. This test monitors asthma severity and measures how well the treatment works. Sometimes more sophisticated tests are needed to quantify your lung function and see how responsive your lungs are to stimuli.
Management
Although there is no cure for asthma, asthma symptoms can be managed by avoiding triggers and taking medications as directed. Your doctor will determine the severity of your or your children’s asthma, based on the impairment of daily life, lung function, how bad the exacerbations are, etc; and decide what medications to start. Interval re-assessments are needed to adjust medications, to control the symptoms while minimizing side effects. This method is called step up / step down.
There are two types of medications for asthma: controller medications and rescue medications. Usually for intermittent asthma, rescue medications – fast acting medications to dilate airways (bronchodilator) are sufficient. If you have to use rescue relief more than twice a week, you need to talk to your doctor. For persistent asthma, controllers are taken on a daily basis to suppress inflammation. These include inhaled corticosteroids, combination inhalers containing a steroid with a long action bronchodilator, or oral medications (Cromolyn, Montelukast, Theophylline, etc). Oral steroids are usually used for acute asthma flares. For those with severe allergic asthma who have failed multiple medications, an injection underneath the skin with Omalizumab (Xolair) that blocks allergy cell activation can be considered.
For self-care, avoidance of asthma trigger is critical. You may monitor your breathing with peak flow at home. Peak flow decrease by 20% from personal best should raise alert. Asthma control test (4-11yr, 12 yo and above) is an easy tool for self- assessment. Notify your doctor is the score is below 19.
Useful linkes:
http://www.aaaai.org/conditions-and-treatments/asthma.aspx